Adaptation and Performance of ESI in the Thai Healthcare System
Thailand officially adopted a modified version of ESI version 4 in 2012, with the primary alteration being a refinement of the "danger zone" vital sign parameters used to identify high-risk patients. To promote national consistency, the Ministry of Public Health (MOPH) subsequently developed the MOPH ED Triage Guideline.


The effective triage of patients in crowded emergency departments (EDs) is a cornerstone of safe and efficient acute care delivery. The Emergency Severity Index (ESI), a five-level triage algorithm developed in the United States, has been widely adopted internationally due to its dual focus on patient acuity and anticipated resource utilization. This report provides a comprehensive analysis of the adaptation, implementation, and performance of the ESI within the unique context of the Thai healthcare system.
Thailand officially adopted a modified version of ESI version 4 in 2012, with the primary alteration being a refinement of the "danger zone" vital sign parameters used to identify high-risk patients. To promote national consistency, the Ministry of Public Health (MOPH) subsequently developed the MOPH ED Triage Guideline, establishing a standardized five-level framework for all hospitals. Alongside this national standard, localized and regional triage systems, such as the Ramathibodi Triage System (RTS) and the Regional 4 Triage System (R4TS), have been developed to better suit specific institutional and regional needs.
Performance analysis based on numerous clinical studies conducted in Thai hospitals reveals a complex picture. While the five-level ESI framework has demonstrated superior accuracy compared to older four-level systems and is a strong predictor of critical outcomes such as mortality and ICU admission, its practical implementation is fraught with challenges. Triage accuracy rates are highly variable and often fall short of international benchmarks, with significant rates of both over-triage and under-triage. Over-triage, the more common error, strains limited resources and exacerbates ED crowding, while under-triage poses a direct threat to patient safety. The system has shown a particularly critical performance gap in pediatric populations, where mistriage rates are unacceptably high.
Key factors influencing triage accuracy include systemic pressures like ED overcrowding, fueled by a high volume of non-urgent presentations, and human factors, most notably the clinical experience of the triage nurse. Research consistently shows that more experienced nurses are significantly more accurate. Concurrently, technological innovation has emerged as a powerful solution. Studies in Thailand have provided robust evidence that mobile ESI applications significantly improve inter-rater reliability and user confidence compared to traditional paper-based methods by reducing cognitive load and ensuring consistent application of the algorithm.
Based on this comprehensive analysis, this report puts forth a series of strategic recommendations aimed at optimizing the triage system in Thailand. These include the national-level promotion and subsidization of validated mobile triage platforms, a redesign of nurse training to focus on clinical reasoning for high-risk populations (elderly and pediatric), the development of a dedicated national pediatric triage guideline, the implementation of a national quality improvement program for triage auditing, and the integration of ESI with Early Warning Scores (EWS) to facilitate dynamic patient reassessment. While Thailand has successfully established a modern triage framework, the path forward requires a concerted effort to bridge the gap between policy and practice through targeted training, technological adoption, and a commitment to continuous, data-driven quality improvement.
The International Standard: A Foundational Overview of the Emergency Severity Index (ESI)
To accurately assess the nuances and implications of the Emergency Severity Index (ESI) adaptations within Thailand, it is imperative to first establish a comprehensive understanding of the standard international ESI algorithm. The ESI is not merely a classification system but a structured clinical decision-making tool designed to function within the chaotic and resource-limited environment of a modern emergency department (ED). Its architecture reflects a sophisticated balance between immediate clinical acuity and the pragmatic prediction of resource needs, a combination that distinguishes it from other prominent international triage systems.
1.1 The Conceptual Framework: Balancing Acuity and Resource Prediction
The ESI is a five-level ED triage algorithm, first developed in the United States in 1998 by emergency physicians Richard Wuerz and David Eitel. Its primary function is to rapidly and reproducibly stratify the heterogeneous population of patients presenting to an ED into five distinct groups based on urgency, from level 1 (most urgent) to level 5 (least urgent). The conceptual model of the ESI is built upon two core pillars: an assessment of the patient's physiological stability and risk of deterioration, and for those patients deemed stable, a prediction of the resources required to reach a clinical disposition (i.e., admission or discharge).
This dual focus on both acuity and resource prediction is the ESI's defining characteristic. It differentiates the ESI from other widely used systems, such as the Australasian Triage Scale (ATS) and the Canadian Triage and Acuity Scale (CTAS), which primarily use presenting symptoms and diagnoses to determine how long a patient can safely wait for physician assessment. By incorporating resource needs, the ESI aims not only to identify the sickest patients for immediate care but also to facilitate operational efficiency and patient flow management for the entire department. The algorithm is intended for use by registered nurses with significant emergency nursing and triage experience, as its application requires a foundation of clinical knowledge to accurately assess stability and anticipate care pathways.
1.2 The Five-Level Acuity Scale: From Resuscitation to Non-Urgent
The ESI framework categorizes patients into five clinically relevant and intuitive levels, providing a common language for communicating patient urgency among healthcare providers.
ESI Level 1 (Immediate): This level is reserved for patients requiring immediate, life-saving intervention to prevent death. These are individuals who are critically unstable, such as those in cardiac arrest, who are unresponsive to stimuli, or who require immediate airway management (e.g., intubation).
ESI Level 2 (Emergency): This category includes patients who are not in immediate peril but are in a high-risk situation that could easily deteriorate, or who present with a time-critical problem. This determination is based on three key criteria: a high-risk presentation (e.g., active chest pain suspicious for cardiac ischemia, signs of a stroke), a confused, lethargic, or disoriented mental state, or severe pain or distress. These patients require urgent evaluation and treatment, typically within minutes.
ESI Level 3 (Urgent): Patients at this level are considered physiologically stable. Their triage level is determined by the prediction that they will require two or more resources to work up their condition and arrive at a disposition. A common example is a stable patient with abdominal pain who will likely need blood tests (one resource) and a CT scan (a second resource).
ESI Level 4 (Non-urgent): These patients are also stable but are anticipated to require only one resource. Examples include a patient with a simple ankle injury needing only an X-ray, or a patient with a simple laceration requiring only sutures.
ESI Level 5 (Minor): This is the least urgent category for stable patients who are predicted to require no resources for their care. Their evaluation typically involves only a history and physical examination by a provider. Examples include patients presenting for a prescription refill, dressing change, or suture removal.
The definition of a "resource" is specific and crucial to the algorithm's application for levels 3, 4, and 5. Resources include laboratory tests (blood, urine), diagnostic imaging (X-rays, CT, ultrasound), IV fluids, IV or IM medications, specialty consultations, and complex procedures like sutures or conscious sedation. Importantly, simple interventions such as oral medications, saline locks, crutches, splints, simple wound care, and prescriptions are explicitly not considered resources.
1.3 The Four-Point Decision Algorithm in Practice
The assignment of an ESI level is not arbitrary but follows a strict, hierarchical algorithm comprising four key decision points. The triage nurse must address these points in sequential order to arrive at the correct classification.
Decision Point A: "Is the patient dying?" The nurse performs a rapid "first look" assessment to determine if the patient requires immediate life-saving intervention (e.g., is apneic, pulseless, unresponsive, or in severe respiratory distress). If the answer is "yes," the patient is immediately categorized as ESI 1, and the algorithm stops.
Decision Point B: "Is this a patient who shouldn't wait?" If the patient does not meet ESI 1 criteria, the nurse then assesses for high-risk indicators. This involves answering three questions: (1) Is this a high-risk situation (e.g., a patient with a history of diabetes presenting with subtle signs of a heart attack)? (2) Is the patient confused, lethargic, or disoriented? (3) Is the patient in severe pain or distress? A "yes" to any of these questions leads to an ESI 2 classification.
Decision Point C: "How many resources will this patient need?" If the patient is stable and does not meet ESI 1 or 2 criteria, the triage process shifts from acuity assessment to resource prediction. Based on the chief complaint, patient history, and a focused physical assessment, the experienced nurse anticipates the number of distinct resources needed to reach a disposition. This determines the assignment to ESI 3 (two or more resources), ESI 4 (one resource), or ESI 5 (no resources). This step is a significant source of subjectivity within the algorithm, as it relies heavily on the nurse's clinical experience and knowledge of institutional care pathways. An inexperienced clinician may struggle to accurately predict the diagnostic workup for an unfamiliar or atypical presentation, which can lead directly to mistriage. This contrasts sharply with systems like CTAS, which rely on more objective lists of presenting symptoms.
Decision Point D: "What are the patient's vital signs?" As a final safety check, a full set of vital signs (heart rate, respiratory rate, blood pressure, oxygen saturation) must be obtained for any patient being considered for ESI 3. The ESI algorithm provides age-specific tables of "danger zone" vital signs. If any of the patient's vital signs fall within these danger zones, the triage nurse must reassess and consider upgrading the patient's acuity to ESI 2. This step functions as a critical safety net, designed to catch patients with subtle signs of physiological instability who may otherwise appear stable. However, its placement late in the algorithm creates a specific vulnerability. A nurse who is rushed or who incorrectly assumes a patient is a clear ESI 4 or 5 might bypass this formal vital sign check, potentially missing a patient with a dangerous but compensated condition like silent hypoxia. Therefore, any modification to these vital sign parameters, as was done in Thailand, represents a high-stakes adjustment to the algorithm's most important objective backstop for stable patients.
Table 1: The Standard Emergency Severity Index (ESI) v.4/v.5 Algorithm
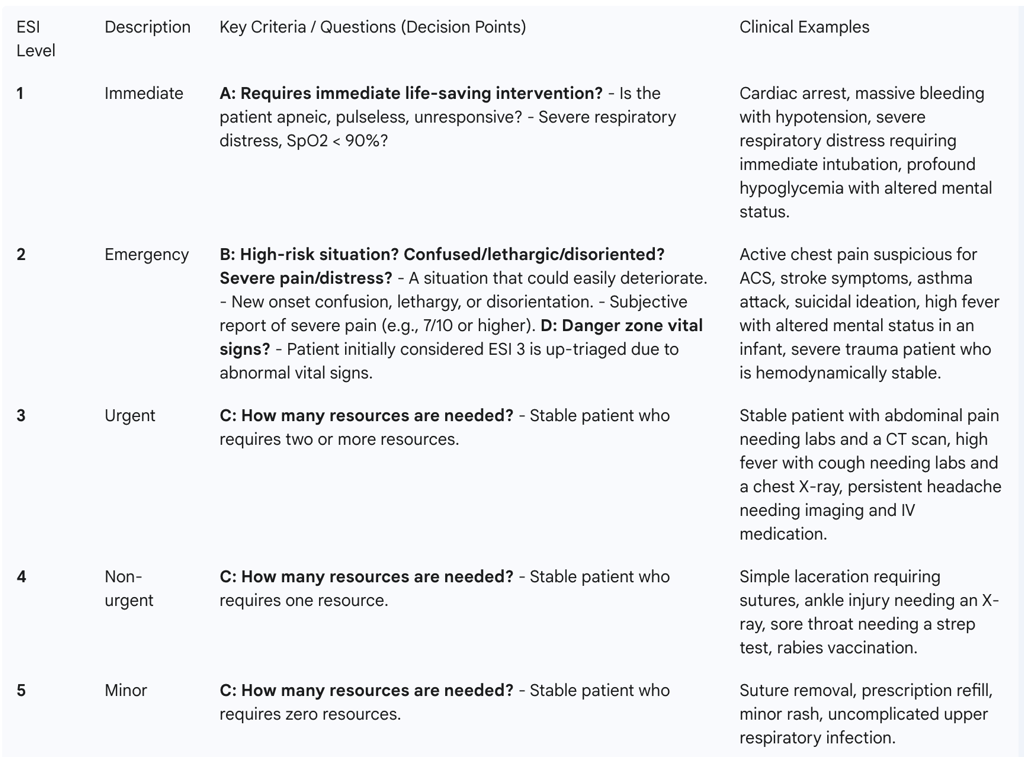

1.4 Special Considerations and Limitations
While the ESI has been validated in numerous studies and settings, its developers and proponents acknowledge specific limitations and populations requiring special consideration. For pediatric patients, whose physiological responses to illness and injury differ significantly from adults, the ESI should be used in conjunction with a rapid visual assessment tool like the Pediatric Assessment Triangle (PAT). The algorithm is explicitly not designed for use in mass casualty incidents or multi-victim trauma events, where specialized triage systems like Simple Triage and Rapid Treatment (START) or its pediatric equivalent, JumpSTART, are the appropriate tools.
Furthermore, despite its widespread use and demonstrated reliability, the implementation of ESI is not immune to error. Studies have shown that mistriage is a common and significant problem. These errors fall into two categories: under-triage, where a patient is assigned a less urgent category than their condition warrants, and over-triage, where they are assigned a more urgent category. Under-triage can lead to critical delays in treatment and adverse patient outcomes, while over-triage leads to the misallocation of limited ED resources, contributing to departmental crowding and potentially delaying care for other, sicker patients. This inherent potential for error underscores the importance of robust training, continuous quality improvement, and careful adaptation when implementing the ESI in a new healthcare system.
The Thai Adaptation: Modifying ESI for a National Context
The adoption of the Emergency Severity Index in Thailand was not a simple replication of the American model but rather a multi-stage process of adaptation, standardization, and localized innovation. This evolution reflects a broader effort within the Thai healthcare system to modernize emergency medical services by implementing an evidence-based, internationally recognized triage standard. The process has been characterized by a top-down push for national uniformity through official guidelines, alongside bottom-up development of institution-specific and regional systems designed to address local needs.
2.1 Official Adoption and the "Modified ESI v.4"
In 2012, the Emergency Medical Committee of Thailand officially announced its adoption of a version of the ESI, specifically a "modified ESI v.4," for nationwide use by trained healthcare providers. This marked a significant policy shift towards a five-level triage system, aligning Thailand with a widely accepted international standard.
The most significant and explicitly documented change in this Thai-modified version was the alteration of the "danger zone of vital signs". These parameters are the objective criteria used at Decision Point D of the ESI algorithm to compel the triage nurse to reconsider an initial ESI 3 classification and potentially up-triage the patient to the higher-acuity ESI 2 level. The rationale provided for this modification was to enhance the tool's efficacy, particularly for pediatric patients. This justification acknowledges that children have distinct physiological responses to illness and that the standard American-derived vital sign thresholds might not be optimally calibrated for the Thai pediatric population. Such a specific, technical change suggests a reactive adaptation, likely driven by clinical experience and a pattern of adverse events where patients initially deemed "stable" later deteriorated because their abnormal vital signs did not meet the original ESI's criteria for up-triage. This modification represents a deliberate attempt to increase the sensitivity of the algorithm's final safety net for patients who do not present with immediately life-threatening or high-risk conditions.
2.2 The MOPH ED Triage Guideline: Forging a National Standard
To ensure consistent application and create a unified standard of emergency care across its diverse network of hospitals, Thailand's Ministry of Public Health (MOPH) developed and disseminated the MOPH ED Triage Guideline. This national guideline represents a crucial top-down effort to move beyond fragmented local practices and establish a common language and methodology for patient triage.
The guideline is explicitly based on international triage systems, referencing both the ESI and the Canadian Triage and Acuity Scale (CTAS), and solidifies the move to a five-level system. Its stated purpose is to create a standardized approach that can link the service levels of different hospitals, from rural community hospitals to tertiary urban centers, ensuring that a patient's acuity level is understood consistently throughout the system. The guideline defines five patient categories using Thai terminology that directly aligns with the principles of the ESI framework :
Level 1: Resuscitation (ผู้ป่วยฉุกเฉินวิกฤต)
Level 2: Emergency (ผู้ป่วยฉุกเฉินมาก)
Level 3: Urgency (ผู้ป่วยฉุกเฉิน)
Level 4: Semi-urgency (ผู้ป่วยกึ่งฉุกเฉิน)
Level 5: Non-urgency (ผู้ป่วยไม่ฉุกเฉิน)
The implementation of the MOPH guideline is designed as a structured quality improvement process. It encourages hospitals to analyze their existing triage problems, provide comprehensive training to personnel, and continuously evaluate performance outcomes, with a specific focus on reducing rates of under-triage and over-triage. This national framework provides the essential scaffolding for a modern, standardized emergency care system.
2.3 Localized and Regional Systems: Ramathibodi and Regional 4 Triage Systems (R4TS)
The national push for standardization coexists with a history of localized innovation at major academic medical centers and, more recently, the development of regionally adapted systems. This dynamic creates a tension between the benefits of a single national standard and the potential for optimized performance through local tailoring.
For example, Ramathibodi University Hospital, a leading tertiary care center in Bangkok, had historically used its own systems, including a four-level "Ramathibodi-nurse triage" system. For pediatric patients, the hospital developed the five-level "Ramathibodi Triage System (RTS)," a computer-based tool that uses chief complaints and vital signs to determine acuity. The development of these bespoke systems highlights the need felt by high-volume, high-acuity centers for tools precisely calibrated to their patient populations and workflows.
More recently, this trend has extended to the regional level with the creation of the Regional 4 Triage System (R4TS). This system was developed by adapting core principles from both ESI and CTAS to better fit the context of hospitals within a specific health region. A 2021 comparative study conducted at Saraburi Hospital yielded compelling results: the locally adapted R4TS demonstrated the highest overall validity (69%) when compared to both standard ESI (65%) and CTAS (63%). This finding suggests that while a national standard is crucial for interoperability, a single, rigid protocol may not be optimally effective across the diverse healthcare landscape of Thailand. The superior performance of R4TS in its local context indicates that the most effective national strategy may be one that provides a common framework (like the MOPH guideline) but allows for structured, evidence-based regional modifications.
2.4 Synergistic Approaches: Integrating ESI with Early Warning Scores (EWS)
Recognizing that any triage system provides only a static, point-in-time assessment of a patient's condition, some Thai researchers and clinicians have pioneered a more dynamic approach by integrating the ESI with Early Warning Scores (EWS). This represents a proactive evolution in triage philosophy, moving beyond the question of "How sick is this patient now?" to also address "What is this patient's likely trajectory?"
One such research and development study created a triage model that combines the standard ESI algorithm with an EWS that assesses key physiological parameters: respiratory rate, heart rate, oxygen saturation, systolic blood pressure, body temperature, level of consciousness, pain score, and fatigue. This hybrid model was found to have high consistency (83.3%) in triage decisions between outpatient and ED nurses and, critically, resulted in no incidents of patient deterioration while waiting for examination. This integration is a sophisticated adaptation that directly addresses a core weakness of all point-in-time triage systems—their inability to account for a patient's dynamic clinical course. By providing a structured framework for ongoing monitoring and clear triggers for reassessment, the ESI-EWS model represents a potential future direction for enhancing patient safety in crowded Thai EDs.
Table 2: Comparison of Standard ESI and Key Thai Triage Adaptations
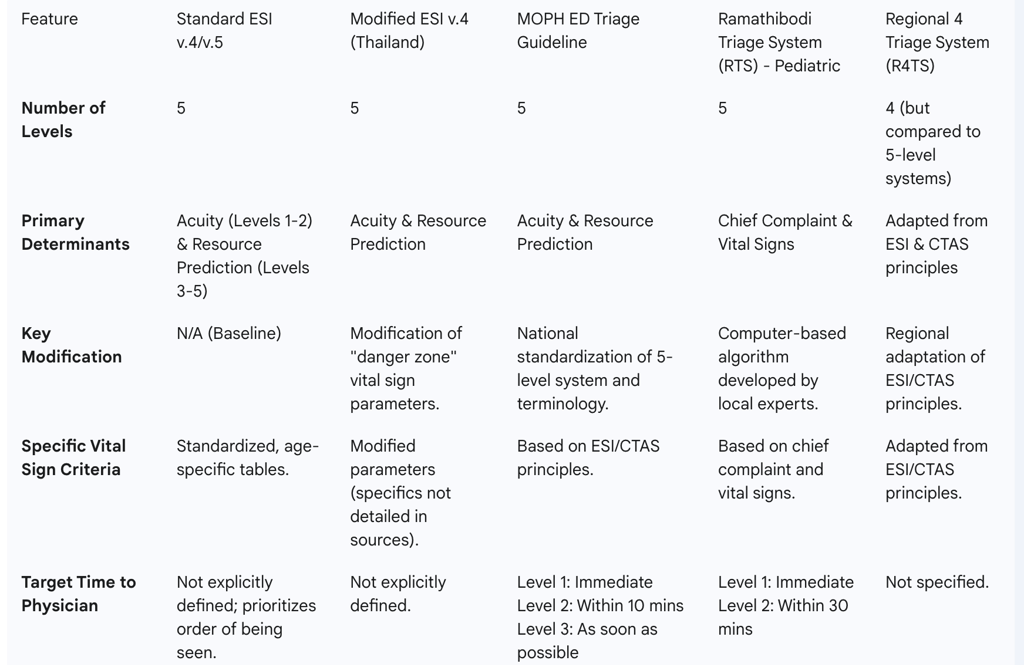
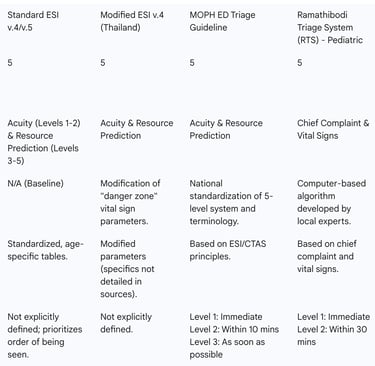
Performance Analysis: Evaluating ESI in Thai Emergency Departments
The ultimate measure of any triage system's value lies in its real-world performance. A robust body of research from hospitals across Thailand provides critical data on the accuracy, comparative effectiveness, and clinical utility of the ESI and its local adaptations. This evidence reveals a system that, while conceptually sound and effective in predicting severe outcomes, faces significant challenges in achieving consistent and accurate implementation across diverse clinical settings and patient populations.
3.1 Accuracy, Validity, and Reliability: A Synthesis of Thai Clinical Studies
Studies evaluating the accuracy of ESI triage in Thai EDs report widely varying results, pointing to inconsistencies in application and performance. A study of triage accuracy among ED nurses found an overall accuracy rate of 67% , while a separate study involving seven tertiary hospitals in the Bangkok Metropolitan Region reported a similar figure of 68.7%. However, performance appears to be lower in specific, high-risk populations; a study focused exclusively on trauma patients found that nurses achieved an accurate triage classification in only 52.4% of cases.
Mistriage, encompassing both over-triage and under-triage, remains a persistent and significant problem. A 2023 retrospective study at Vajira Hospital found that while triage was correct in 69.1% of cases, there was a substantial over-triage rate of 26.0% and an under-triage rate of 4.9%. These figures highlight a tendency among clinicians to err on the side of caution. When faced with uncertainty, triage nurses appear more likely to assign a higher, "safer" acuity level (over-triage) than a lower, "riskier" one. While this may seem like a prudent strategy to avoid missing a critically ill patient, it is not a benign error. A high rate of over-triage diverts limited resources—such as monitored beds, nursing attention, and physician time—to less acute patients, thereby contributing to ED crowding and increasing wait times for all, including the next patient who may be truly critical.
These reported mistriage rates often struggle to meet established international safety benchmarks, which typically recommend an under-triage rate of less than 5% and an over-triage rate of no more than 25-35%. Of particular concern are reports from pre-hospital dispatch centers in Thailand, where under-triage rates have been observed to be as high as 40-42%, posing a substantial risk to patient safety by delaying the dispatch of appropriate emergency medical services.
3.2 Comparative Effectiveness: ESI vs. Local and International Triage Systems
Comparative studies conducted within Thailand provide valuable, locally-derived evidence on the relative strengths of the ESI framework compared to both older local systems and other international standards.
A landmark study at Ramathibodi Hospital provided powerful evidence supporting the national transition to a five-level system. The research directly compared the performance of the five-level ESI against the hospital's incumbent four-level nurse triage system. The results were definitive: the five-level ESI was significantly more accurate in its ability to predict the need for life-saving interventions. This was demonstrated by a markedly superior area under the receiver operating characteristic (ROC) curve—a statistical measure of diagnostic accuracy—of 92.2% for ESI versus 81.3% for the four-level system. This finding validates the move toward a more granular five-level system, as the additional level of stratification (specifically, the ability to separate zero-resource ESI 5 patients from one-resource ESI 4 patients) adds tangible clinical value in discriminating patient severity and managing departmental flow.
In other contexts, however, locally adapted systems have shown the potential to outperform international standards. A study at Saraburi Hospital compared the regionally developed Regional 4 Triage System (R4TS) with both ESI and the Canadian Triage and Acuity Scale (CTAS). The R4TS achieved the highest overall validity score (69.0%), surpassing both ESI (65.0%) and CTAS (63.0%). This suggests that while ESI provides a robust framework, systems that are thoughtfully adapted to local patient demographics, case mixes, and resource availability may achieve superior performance.
The ESI has also proven to be a highly effective tool for specific clinical presentations. In a study of suspected sepsis patients at a tertiary care hospital in Khon Kaen, the ESI's accuracy in predicting in-hospital mortality and ICU admission was comparable to that of the National Early Warning Score (NEWS). Critically, however, classifying patients as ESI level 1 or 2 demonstrated the highest sensitivity (96.7%) for predicting in-hospital mortality, establishing it as an exceptionally valuable screening tool for identifying high-risk sepsis patients at the front door of the ED.
3.3 Predictive Value for Clinical Outcomes: Mortality, ICU Admission, and Length of Stay
Across multiple Thai studies, the assigned ESI level has been shown to be a strong and reliable predictor of key clinical outcomes. There is a clear and consistent correlation between ESI acuity level and the likelihood of hospital admission, admission to the intensive care unit (ICU), and in-hospital mortality. Patients triaged as ESI 1 and 2 consistently have the highest rates of admission and mortality, confirming the tool's validity in identifying the most severely ill patients.
The Emergency Department Length of Stay (EDLOS) is another critical metric that correlates significantly with ESI level; higher acuity patients predictably require more extensive workups and stabilization, leading to longer stays in the ED. More than just an operational metric, EDLOS has been identified as a crucial patient safety indicator in the Thai context. A large cross-sectional study found that an EDLOS exceeding four hours was an independent and significant risk factor for 72-hour in-hospital mortality among patients triaged as ESI 2 and ESI 3. This finding highlights the life-threatening consequences of ED crowding and delays in moving admitted patients to inpatient beds.
3.4 A Critical Gap: The Challenge of Pediatric Triage Accuracy
While the ESI has demonstrated its value in adult populations, its performance in pediatric triage within the Thai context is a source of significant concern. A pivotal study conducted at Songklanagarind Hospital to assess the validity and reliability of the modified ESI v.4 for pediatric patients found the tool to be performing poorly.
The results of this study were alarming. Triage nurses and a research physician assigned the same ESI level in only 43.84% of cases, indicating low inter-rater reliability. More critically, the nurses' triage classifications resulted in an under-triage rate of 30.85% and an over-triage rate of 25.31%. An under-triage rate of this magnitude is a major patient safety failure, as it means nearly one-third of children were assigned a lower acuity level than their condition warranted, placing them at risk for delayed treatment. This poor performance strongly suggests that the modifications made to the ESI v.4, which focused on vital signs, were likely developed with adult physiology in mind and are fundamentally insufficient to address the unique challenges of pediatric assessment. Children often compensate physiologically for severe illness until they deteriorate abruptly. The standard ESI protocol acknowledges this by recommending the supplemental use of the Pediatric Assessment Triangle (PAT). The results from the Songklanagarind study imply that either this recommendation is not being implemented effectively or that the combination of the Thai-modified ESI and the PAT is still inadequate, representing a critical safety gap that requires urgent, targeted intervention.
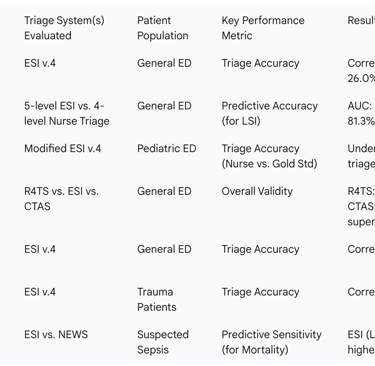
Table 3: Summary of Performance Metrics from Key Thai Triage Studies
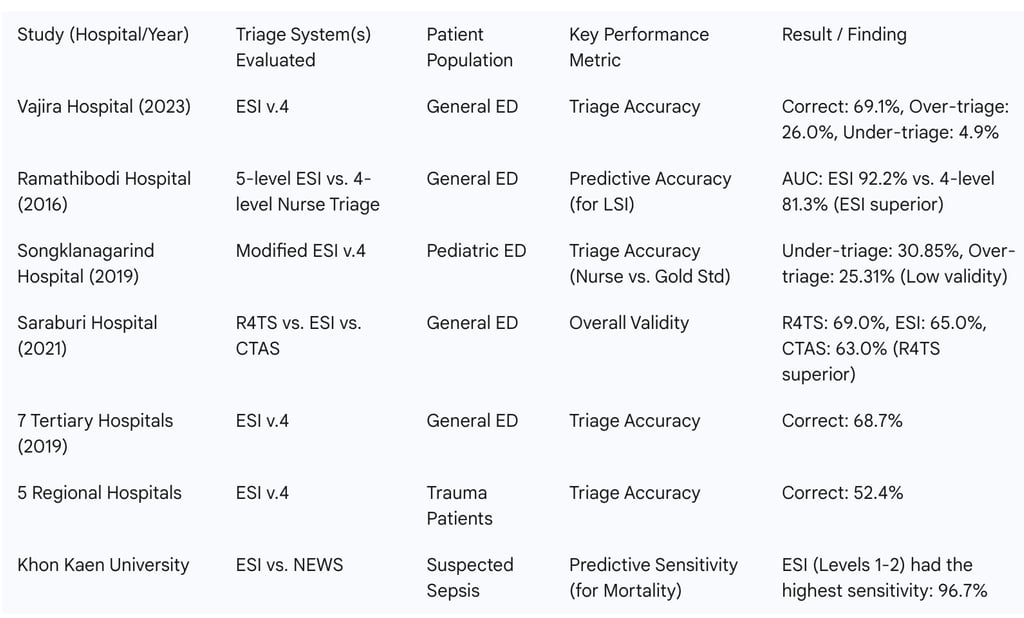
Implementation in Practice: Challenges, Human Factors, and Innovations
The performance of a triage algorithm is not determined solely by its design but is profoundly influenced by the complex interplay of the environment in which it is used, the skills of the clinicians who apply it, and the tools available to support them. In Thailand, the implementation of the ESI has been shaped by systemic pressures like ED overcrowding, critical human factors such as nurse experience, and the emergence of technological innovations that promise to mitigate some of these persistent challenges.
4.1 Systemic Pressures: ED Overcrowding and Resource Constraints
A fundamental challenge confronting the Thai emergency care system, and by extension its triage processes, is the immense pressure of ED overcrowding. A report from the National Institute of Emergency Medicine of Thailand indicated that a staggering 60% of patients who present to EDs do not have conditions that require urgent treatment. This high volume of low-acuity patients consumes physical space and clinical attention, creating a chaotic and high-pressure environment that makes the primary task of triage—identifying the critically ill amidst the crowd—exponentially more difficult.
This phenomenon is not unique to Thailand; ED overcrowding is an international crisis linked to significant negative consequences, including delays in time-sensitive care, increased risk of medical errors, adverse patient outcomes, and higher mortality rates. In Thai hospitals, this pressure manifests as prolonged EDLOS, which is exacerbated by system-wide issues such as limited inpatient bed availability. As established, this is not merely an operational inconvenience; prolonged EDLOS is a direct predictor of increased mortality. This reality creates a reinforcing feedback loop: overcrowding contributes to triage errors, and the most common error, over-triage, misallocates resources and worsens crowding, further increasing the risk for all patients in the department. Breaking this cycle requires a highly accurate and efficient triage system, yet the very conditions of overcrowding make achieving such accuracy a formidable challenge.
4.2 The Human Element: Impact of Nurse Experience and Training on Triage Accuracy
The ESI algorithm is not a self-executing protocol; its accuracy is fundamentally dependent on the clinical judgment, knowledge, and experience of the triage nurse. Research conducted in Thailand consistently underscores the critical role of experience. A study across seven tertiary hospitals found that nurses with six to ten or more years of ED experience had significantly lower rates of both over-triage and under-triage when compared to their less experienced colleagues with only one to five years of experience. Based on these findings, the study recommended that nurses appointed to triage roles should possess a minimum of five years of ED experience to minimize triage errors.
The characteristics of the patients themselves also interact with nurse experience to influence accuracy. Multiple studies have identified specific patient populations that are at higher risk for mistriage. Elderly patients (over 65 years of age) are frequently under-triaged, a dangerous error pattern likely due to their often atypical or subtle presentations of serious illness. Conversely, patients presenting with trauma are more likely to be over-triaged, as nurses may defensively assign a higher acuity level in the face of dramatic injuries, even without physiological instability.
One of the most perplexing findings to emerge from the Thai research is the "training paradox." A large study in the Bangkok Metropolitan Region found, counterintuitively, that under-triage was more frequent among nurses who had successfully passed a standardized triage training program than among those who had not. While the study itself does not offer an explanation for this result, it is unlikely to be an indictment of training as a concept. Instead, it likely points to confounding variables and the limitations of standardized education versus tacit clinical knowledge. It is plausible that less experienced nurses—who are already known to be less accurate—are also the most likely to have recently completed a mandatory training course. The data may simply be showing that a novice nurse with training is still less accurate than a veteran nurse without recent formal training, making experience the dominant predictive factor. Alternatively, standardized training might foster a rigid, algorithmic approach that is less effective for interpreting the ambiguous or atypical presentations common in high-risk groups like the elderly. This finding suggests that training should not be abandoned but rather redesigned to focus more on clinical reasoning, simulation of complex cases, and structured mentorship.
4.3 A Digital Solution: The Proven Efficacy of Mobile ESI Applications
In response to the challenges of inconsistent application and cognitive demands of paper-based triage, mobile health technology has emerged as a highly effective solution in the Thai context. A number of studies have evaluated the use of mobile applications designed to guide clinicians through the ESI algorithm.
A pivotal study at Ramathibodi Hospital provided clear evidence of the superiority of this approach. It directly compared a mobile ESI application against the traditional paper-and-handbook method. The results demonstrated that the mobile platform led to significantly better inter-rater reliability, a measure of consistency between different clinicians. The lowest kappa statistic (a measure of agreement) in the mobile app group was 0.84 (indicating "almost perfect" agreement), whereas the highest kappa in the paper-based group was only 0.69 (indicating "substantial" agreement). Furthermore, both medical students and experienced emergency physicians reported feeling more confident in their triage decisions when using the mobile application.
These findings have been supported by other research in Thailand, which confirms that mobile triage apps are more effective than paper-based methods in improving both accuracy and reliability, and can help reduce the rates of both under-triage and over-triage. The success of these applications suggests that a primary failure point in manual triage is not necessarily a lack of knowledge, but rather the cognitive overload experienced by nurses who must recall and apply a complex, multi-step algorithm under immense time pressure. A well-designed mobile application mitigates this by structuring the decision-making process. It forces a sequential, step-by-step application of the algorithm, presents criteria clearly, and automates calculations, thereby reducing the cognitive burden and ensuring a more standardized and consistent process for every patient. This indicates that one of the most impactful interventions to improve triage accuracy is the adoption of better-designed tools that simplify execution.
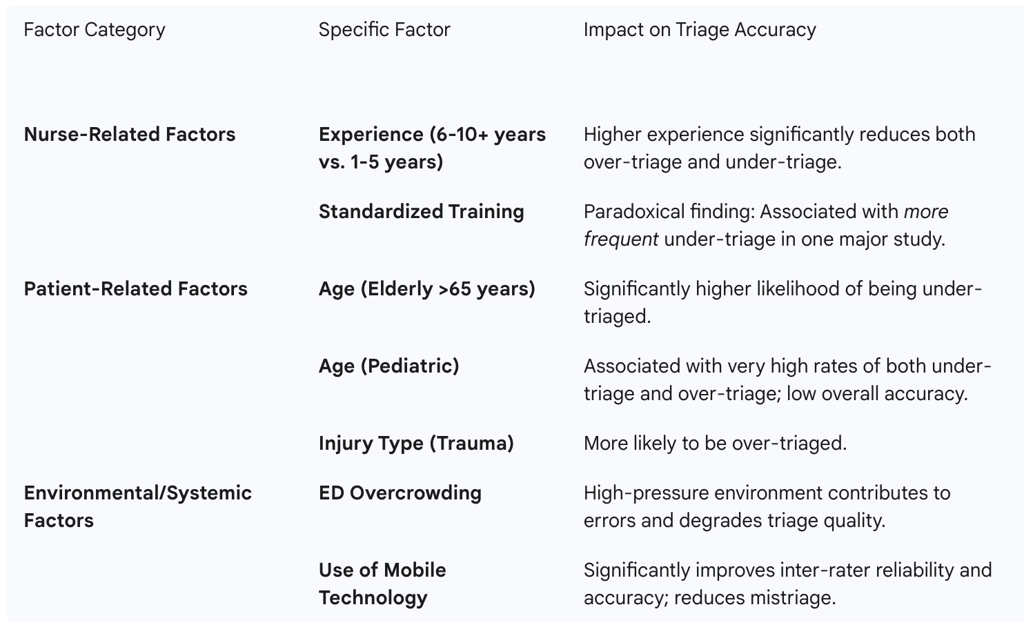
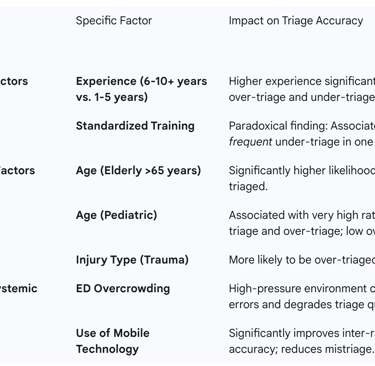
Table 4: Identified Factors Influencing Triage Accuracy in Thai EDs
Synthesis and Strategic Recommendations
The comprehensive analysis of the Emergency Severity Index's journey in Thailand—from its initial adaptation to its performance in diverse clinical settings—reveals a healthcare system actively engaged in modernizing its emergency care infrastructure. The national commitment to a standardized, five-level triage system is a foundational strength. However, significant gaps between policy and practice persist, evidenced by inconsistent triage accuracy, critical challenges in special populations, and the ongoing strain of ED overcrowding. To bridge these gaps and optimize the system for enhanced patient safety and efficiency, a series of strategic, evidence-based actions are required.
5.1 An Expert Assessment of Thai ESI Adaptations: Strengths and Weaknesses
A holistic assessment of the ESI's implementation in Thailand highlights several key strengths and persistent weaknesses.
Strengths:
National Standardization: The adoption of a modified ESI v.4 and the development of the MOPH ED Triage Guideline represent a major systemic strength, creating a common framework and language for patient acuity across the country.
Proven Predictive Validity: In the Thai context, the ESI has been repeatedly validated as an effective tool for predicting critical patient outcomes, including the need for life-saving intervention, ICU admission, and in-hospital mortality.
Commitment to Innovation: The healthcare system has shown a clear willingness to innovate and improve upon the standard model. This is evidenced by the exploration of regionally tailored systems like R4TS, the integration of ESI with Early Warning Scores, and the robust investigation of mobile health technologies.
Weaknesses:
Inconsistent Accuracy: The most significant weakness is the wide variability and often suboptimal rates of triage accuracy in practice. High rates of both over-triage and under-triage indicate a persistent gap between the algorithm's design and its real-world application.
Critical Failure in Pediatrics: The current modified ESI v.4 has been shown to have low validity and reliability in children, resulting in unacceptably high mistriage rates that pose a direct threat to pediatric patient safety.
Unresolved Implementation Challenges: Systemic issues, particularly ED overcrowding and the variable impact of nurse experience and training, continue to undermine the effectiveness of the triage process.
Potential for Suboptimal Standardization: The superior performance of a regionally adapted system (R4TS) in one study raises questions about whether a single, rigid national standard is the most effective approach for a country with diverse regional healthcare needs and resources.
5.2 Pathways to Optimization: Recommendations for Enhancing Triage Accuracy and Efficiency
Based on the synthesized evidence, the following strategic recommendations are proposed to address the identified weaknesses and build upon the existing strengths of the Thai triage system.
Recommendation 1: Mandate and Subsidize the Adoption of Validated Mobile Triage Platforms. The evidence from Thai hospitals is unequivocal: mobile ESI applications lead to significantly higher inter-rater reliability, improved accuracy, and greater user confidence compared to paper-based methods. By structuring the decision-making process and reducing cognitive load, these tools directly address a primary failure point in manual triage. The Ministry of Public Health should therefore prioritize a national transition to digital triage platforms, potentially through subsidizing the adoption of validated software in public hospitals.
Recommendation 2: Redesign Triage Training to Focus on Clinical Reasoning and High-Risk Populations. The "training paradox" suggests that simple algorithmic training is insufficient. Training programs should be redesigned to de-emphasize rote memorization and focus instead on developing higher-order clinical reasoning skills. This should involve high-fidelity simulation-based training that challenges nurses with ambiguous and atypical presentations, particularly those common in high-risk groups like the elderly and trauma patients. Furthermore, to leverage the proven impact of experience, a period of structured mentorship and supervised practice should be a mandatory component of certification for any nurse newly assigned to a triage role.
Recommendation 3: Develop and Validate Specific Pediatric ESI Guidelines for Thailand. The demonstrated failure of the current modified ESI v.4 in pediatric populations constitutes a critical patient safety gap that must be addressed urgently. A national task force, comprising pediatric emergency medicine specialists, experienced nurses, and researchers, should be convened to develop and validate a dedicated Thai Pediatric Triage (TPT) guideline. This effort could build upon existing local innovations like the Songklanagarind Pediatric Triage (SPT) model and should more formally and rigorously integrate the use of the Pediatric Assessment Triangle (PAT) into the triage algorithm.
Recommendation 4: Implement a National Triage Quality Improvement (QI) Program. To drive continuous improvement, a standardized national Triage QI Program should be established. This would require all hospitals to regularly audit a sample of their triage decisions, comparing the initial ESI level against final disposition, resource utilization, and patient outcomes. The program would generate standardized data on institutional and regional rates of under-triage and over-triage, allowing for the identification of local error patterns and the implementation of targeted interventions.
Recommendation 5: Integrate ESI with Early Warning Scores (EWS) for Dynamic Re-triage. To transition from static to dynamic risk assessment, the MOPH should promote the adoption of integrated ESI-EWS protocols, as explored in recent Thai research. This would create a system for the continuous or scheduled monitoring of waiting room patients, with clear EWS-based triggers for formal nurse reassessment. Such a system would provide a crucial safety net to identify patients who deteriorate after their initial triage assessment, directly mitigating the risks associated with long wait times in crowded EDs.
5.3 Agenda for Future Research: Unanswered Questions and Next Steps
While existing research provides a strong foundation for action, several key questions remain unanswered. A targeted research agenda is necessary to guide the next phase of triage system optimization in Thailand.
Conduct a multi-center, prospective study specifically designed to investigate the "training paradox." This study should control for nurse experience to isolate the true effect of current training programs and evaluate the effectiveness of redesigned, simulation-based training curricula.
Perform a large-scale, national validation study of the MOPH ED Triage Guideline. This would establish national performance benchmarks, quantify regional variations in accuracy, and provide a robust dataset for future refinements of the guideline.
Launch a multi-center, randomized controlled trial to evaluate the clinical and economic impact of implementing mobile ESI applications versus paper-based methods across different hospital settings (e.g., tertiary, regional, and community hospitals).
Further develop and validate the Regional 4 Triage System (R4TS) and other regional adaptations in broader settings to determine if a flexible framework allowing for evidence-based local modifications is superior to a single national standard.
Investigate the specific factors contributing to the high rate of under-triage in the pre-hospital setting and develop targeted interventions for emergency dispatchers.
Conclusion
The adoption and adaptation of the Emergency Severity Index in Thailand represent a significant and successful step in the modernization of the nation's emergency medical services. The country has successfully established a standardized, five-level conceptual framework that has proven its validity in predicting patient outcomes and prioritizing care. However, the journey from policy adoption to consistent, high-quality execution at the bedside is ongoing. The system currently faces significant challenges related to implementation fidelity, evidenced by variable accuracy rates, persistent problems with mistriage, and a critical performance deficit in pediatric care. The path to overcoming these obstacles and fully realizing the potential of the ESI lies in a multi-pronged strategy that embraces technological innovation, fundamentally redesigns clinical training, develops tailored solutions for high-risk populations, and fosters a culture of continuous, data-driven quality improvement. By addressing these areas with strategic focus and investment, the Thai healthcare system can build upon its strong foundation to create a truly world-class emergency triage system that enhances both patient safety and operational efficiency.
